Evelyn’s Story: A prenatal diagnosis and fetal monitoring leads to a successful heart transplant at 6 months
Meet Evelyn
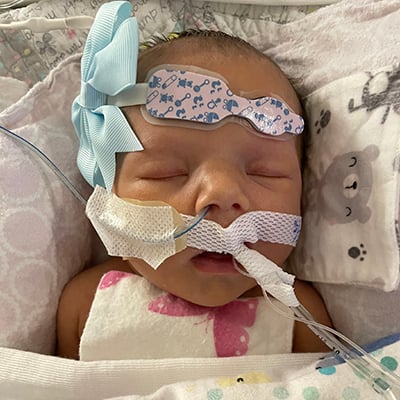
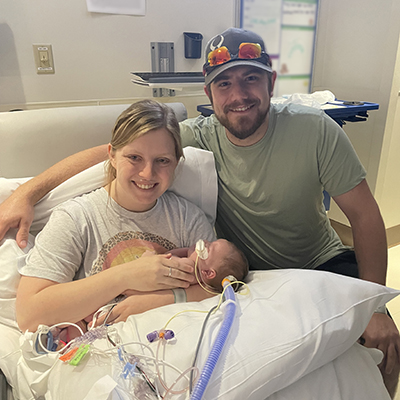
Hannah spent her 27th birthday — and her daughter, Evelyn’s 6-month birthday — at Children’s Mercy, waiting. And waiting. And waiting.
Evelyn was in the operating room getting a new heart. Hannah was with her husband, Trey, passing the 12-hour surgery time by sanitizing Evelyn’s toys and moving them to her post-op room. Late at night, they got word the surgery was successful: They could sneak in a birthday visit before the day was over. “We had this tradition of her wearing pigtails into the OR,” Hannah said. “She was lying there peacefully with her little pigtails intact!”
It was the best birthday gift they could have imagined, and it all began in the Elizabeth J. Ferrell Fetal Health Center (FHC) at Children’s Mercy.
Comprehensive care for mom and baby
The FHC’s multidisciplinary team cares for around 400 families with high-risk pregnancies a year. Established in 2010, the center includes maternal-fetal medicine physicians, nurse practitioners, nurse coordinators, genetic counselors, social workers, neonatologists and other fetal specialists, all in support of parents expecting medically complex babies.
“Even though moms come here for their babies, we are also very focused on the mom’s safety, the mom’s experience, and how the mom is coping,” said Laura Vricella, MD, FACOG, FHC Medical Director. “The prenatal team are the champions of women’s care from the time they come to the FHC through the postpartum period. We all have a really strong bond with our patients.”
Hannah’s local care team transferred her to the FHC after they saw some abnormalities on Evelyn’s 20-week anatomy scan. The FHC diagnosed Evelyn prenatally with critical aortic stenosis, a narrowing of the aorta that restricts blood flow. Hannah had been born with a mild version of aortic stenosis, herself.
“Fetuses whose hearts are formed differently can face additional risks, even during the pregnancy, because of the way the blood flow through the baby’s body is altered,” said Dr. Vricella. “That’s why we watch these pregnancies so carefully.”
At around 26 weeks, Hannah and Trey began driving two and a half hours to the FHC from La Plata, Mo., every week for monitoring. Their appointments included prenatal care for Hannah and a range of fetal tests for Evelyn.
“We do a weekly ultrasound called a biophysical profile, looking at the baby's behavior in utero to tell us if the baby is stressed out,” said Hannah McDaniel, BSN, RNC-OB, FHC Fetal Surgery Program Coordinator. “And then we place a fetal monitor on mom, listen to the baby’s heart rate, monitor if contractions are happening and see what the baby can tell us at that point in time.”
The FHC brought in the teams Evelyn would need after delivery to develop a cooperative plan to address her heart differences. The Ward Family Heart Center team knew they’d have to assess Evelyn quickly at birth and collaborate with their interventional cardiologist colleagues (and possibly the Brendan Tripp Elam Transplant Center) to carve a path forward for their tiny new patient. Meanwhile, the FHC also helped Hannah navigate her own health challenges during the pregnancy, including gestational diabetes.
Care continues after delivery day

In May 2023, Evelyn was born at 39 weeks by C-section in the cardiac operating room.
“For babies with the most complicated hearts, even delivering in the FHC isn't close enough to our cardiac team,” said Dr. Vricella. “So we deliver in the part of the hospital where the baby will get immediate heart care. The maternal-fetal medicine doctors and the neonatologists partner to determine if it's a safe thing for mom to do, and that everything else that mom and the baby need can still be delivered safely.”
After birth, Evelyn immediately underwent an urgent atrial septostomy in the Cardiac Catheterization Lab to boost her heart’s blood flow. The procedure also made it clear that Evelyn had critical aortic stenosis and severe left ventricular dysfunction. More surgery wouldn’t be enough. She needed a heart transplant.
Hannah recovered from her C-section in the FHC, where she was closely watched for wound healing, anemia and any signs of infection. “A mom being able to access her own care at the same hospital where her baby is hospitalized is a huge benefit,” said Dr. Vricella. “We are able to keep moms safe from some of those severe complications that can happen in any pregnancy.”
At 5 days old, Evelyn had a medical hybrid surgery that would give her the best chance of staying strong until a donor heart could be found. It was a scary day: She had complications during the procedure and had to have CPR, but she pulled through.
The FHC was there for Hannah with holistic postpartum care just downstairs from Evelyn’s hospital room. In addition to medical attention, the FHC offers new moms lactation services and mental health resources, including depression and anxiety support before and after birth.
“We keep a really close eye on these moms,” said the FHC’s Heidi Garcia, APRN, MSN, WHNP-BC. “I always tell them this is a different experience, and you’re facing more challenges with a hospitalized [newborn.] So I want to check in on both your mental and physical health.”
Waiting for a new heart together

Evelyn is one of the youngest patients Children’s Mercy has ever evaluated for transplant: She was listed at only 10 days old at 1A status, the highest priority. She stayed in the Cardiac Intensive Care Unit (CICU), where the team could support her as she waited for a new heart. The goal: Go into transplant day as healthy and active as possible, all the while never knowing if and when it would arrive.
Hannah took time off from her job as a special education teacher and moved into the Ronald McDonald House. Trey drove to Kansas City every weekend. “It was a privilege: I got to stay with Evelyn and be really involved in all her therapies and rounds,” said Hannah, who continued to get follow-up care from the FHC through that July.

Finally, in November 2023, it was time for that extraordinary birthday gift: The call came in. A heart was ready. The transplant surgery went well, and although Evelyn had a few minor complications afterward, nothing held her back for long.
With her new heart, Evelyn slowly gained stamina. By the holidays, Evelyn moved out of intensive care to a regular medical/surgical unit. In early 2024, Evelyn was discharged, and the family stayed at the Ronald McDonald House so they could attend all their follow-up appointments easily. In February 2024, the family got to go home and learn to live life with a new baby — with an even newer heart.
They traveled back to Kansas City for follow-ups every two weeks, then every month as their need for appointments tapered. She’s continued to adjust to her new heart well and has remained healthy since her transplant. Evelyn is now almost 3 years old and loves to color and play outside. “She’s loud, she’s sassy, she’s opinionated in all the best ways,” said Hannah.
Evelyn will start preschool in the fall, but first she has a new role to step into: Big sister. She’ll be joined by a little brother in May. Hannah went back to her trusted team at the FHC for an uneventful prenatal check-up earlier this year. The FHC team was happy to see her, but even happier their services wouldn’t be needed this time. Hannah’s second pregnancy has been uncomplicated, and she has been able to get her prenatal care close to home.
“We often say we get to be ‘their person,’” said Hannah McDaniel of the relationships they form with FHC patients. “I consider it a blessing to be there for patients on some of their most joyous days and a privilege to walk through some of their toughest moments, too. Hannah made a lasting impression on me!”